| Reactivity | Hu, Mu, Rt, Po, Bv, Ma, Pm, ChHaSpecies Glossary |
| Applications | WB, Simple Western, DB, ELISA, Flow, Func, ICC/IF, IHC, PAGE, B/N, ChIP, CyTOF-ready, Dual ISH-IHC, ELISA(Cap), KO, Mycoplasma |
| Clone | 76B357.1 |
| Clonality | Monoclonal |
| Host | Mouse |
| Conjugate | Unconjugated |
| Format | BSA Free |
| Concentration | 1.0 mg/ml |
| Immunogen | This TLR4 Antibody (76B357.1) was developed against a portion of amino acids 100-200 of human TLR4 (NP_612564). |
| Predicted Species | Baboon (100%), Chinese Hamster (100%). Backed by our 100% Guarantee. |
| Isotype | IgG2b Kappa |
| Clonality | Monoclonal |
| Host | Mouse |
| Gene | TLR4 |
| Purity | Protein G purified |
| Innovator's Reward | Test in a species/application not listed above to receive a full credit towards a future purchase. |
| Dilutions |
|
|
| Theoretical MW | 95.7 kDa. Disclaimer note: The observed molecular weight of the protein may vary from the listed predicted molecular weight due to post translational modifications, post translation cleavages, relative charges, and other experimental factors. |
|
| Agonist | ||
| Antagonist | ||
| Reviewed Applications |
|
|
| Publications |
|
| Storage | Store at 4C short term. Aliquot and store at -20C long term. Avoid freeze-thaw cycles. |
| Buffer | PBS |
| Preservative | 0.05% Sodium Azide |
| Concentration | 1.0 mg/ml |
| Purity | Protein G purified |
| Images | Ratings | Applications | Species | Date | Details | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
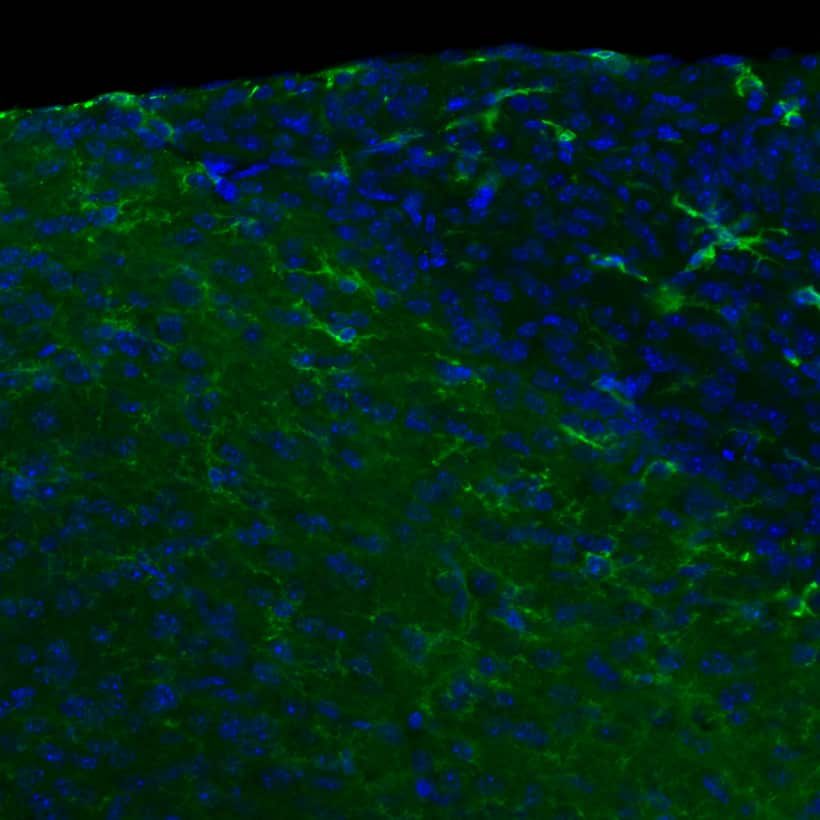
Enlarge |
reviewed by:
Verified Customer |
IHC -Frozen | Mouse | 05/25/2017 |
Summary
Comments
|
||||||||

Enlarge |
reviewed by:
Hayk Simonyan |
IHC | Mouse | 05/16/2017 |
Summary
|
||||||||

Enlarge |
reviewed by:
Aileen Keating |
WB | Other | 05/12/2016 |
Summary
|
||||||||
-(01-mg)_NB100-56566_9196.jpg)
Enlarge |
reviewed by:
Liyong Zhang |
WB | Mouse | 08/07/2014 |
Summary
|
||||||||

Enlarge |
reviewed by:
Courtney Kurtz |
WB | Other | 08/11/2011 |
Summary
|
Secondary Antibodies |
Isotype Controls |
Research Areas for TLR4 Antibody (NB100-56566)Find related products by research area.
|
|
PAMPs and DAMPs: What is the Same and What is Different About These Molecules? By Victoria OsinskiWhat are PAMPs and DAMPsInflammation results from stimuli signaling damage or infection. The immune system inflammatory response can be beneficial or harmful depending on the type and duration of ... Read full blog post. |
|
How To Identify B Cell Subsets Using Flow Cytometry By Victoria OsinskiUsing Flow Cytometry to Identify B Cell SubsetsIdentifying cellular subsets by flow cytometry requires careful and thorough planning in order to ensure the correct subset of cells are identified... Read full blog post. |
|
Lipopolysaccharide from gut microbiome localizes in human atherosclerotic plaques and promotes TLR4-mediated oxidative stress By Jamshed Arslan, Pharm. D., PhD. Atherosclerosis is a chronic inflammatory condition in which plaques of fats and other substances slowly buildup on the inner walls of arteries to restrict blood flow. In atheroscle... Read full blog post. |
|
Toll-like receptors in the intestinal epithelial cells By Jamshed Arslan, Pharm. D., PhD. Toll-like receptors (TLRs) are microbe-sensing proteins that act as first responders to danger signals. TLRs help the intestinal epithelial cells (IECs) recognize commensal bacteria ... Read full blog post. |
|
The role of STING/TMEM173 in gamma and encephalitis Herpes Simplex Virus (HSV) Stimulator of interferon genes (STING), also known as TMEM173, promotes the production of the interferon’s IFN-alpha and IFN-beta. STING possesses three functional domains: a cytoplasmic C-terminal tail, a central globular domain, and four N-... Read full blog post. |
|
TRIF/TICAM1 and mitochondrial dynamics in the innate immune response TRIF, also known as toll like receptor adaptor molecule 1 or TICAM1, is known for its role in invading foreign pathogens as part of our innate immune response. TRIF/TICAM1 is a TIR-domain adaptor protein (toll/interleukin-1 receptor) that interacts... Read full blog post. |
|
The role of TLR4 in breast cancer Toll like receptors (TLRs) are highly conserved proteins that are first known for their role in pathogen recognition and immune response activation. In order to elicit the necessary immune response in reaction to a foreign pathogen, TLRs trigger cy... Read full blog post. |
|
cIAP2 - balancing cell death and cell survival The inhibitor of apoptosis proteins (IAPs) are important regulators of cell death and inflammation. The cellular inhibitor of apoptosis protein 2 (cIAP2) contains three Baculovirus IAP repeat (BIR) domains, a Ubiquitin associated (UBA) domain, and ... Read full blog post. |
|
TLR4 - A Guardian of Innate Immunity Toll-like receptor 4 (TLR4) belongs to the family of Toll-like receptors (TLR), and plays a main role in pathogen recognition and innate immunity system activation. The TLR family members are highly conserved proteins that all contain a high degree of... Read full blog post. |
|
IRAK4: The "master IRAK" critical for initiating immune responses IRAK4, also known as Interleukin-1 receptor-associated kinase 4, is a serine/threonine-protein kinase that plays a critical role in initiating innate and adaptive immune responses against foreign pathogens. It activates NF-kappaB in both Toll-like rec... Read full blog post. |
The concentration calculator allows you to quickly calculate the volume, mass or concentration of your vial. Simply enter your mass, volume, or concentration values for your reagent and the calculator will determine the rest.
5 | |
4 | |
3 | |
2 | |
1 |
| Verified Customer 05/25/2017 |
||
| Application: | IHC -Frozen | |
| Species: | Mouse |
| Hayk Simonyan 05/16/2017 |
||
| Application: | IHC | |
| Species: | Mouse |
| Aileen Keating 05/12/2016 |
||
| Application: | WB | |
| Species: | Other |