 |
By Jamshed Arslan, Pharm. D., PhD.
Coronaviruses are a family of enveloped RNA viruses. Some family members circulate in human populations, but others like severe acute respiratory syndrome coronavirus (SARS-CoV) are transmitted from animals to humans. A new strain of coronaviruses called novel coronavirus (nCOV) or SARS-CoV-2 is also transmitted zoonotically. SARS-CoV-2 has caused a global infectious disease called COVID-19. A person catches this notorious illness when he/she comes in contact with respiratory droplets from an infected person. SARS-CoV-2 in cough or sneeze droplets can survive on surfaces for several days. The most common symptoms of COVID-19 are dry cough, fever, tiredness and difficulty breathing. Good news is that 80% of the infected people recover without any special treatment, but sadly, we do not have any approved antiviral drug or vaccine against SARS-CoV-2. Similar to the strategies adopted during the SARS epidemic of 2002/2003, authorities are trying to halt COVID-19 by travel restrictions and patient isolation. However, an antiviral breakthrough might be our best bet against the COVID-19 pandemic.
Coronaviruses use their spike (S) protein to enter the target cell. The S protein binds to a cellular receptor to facilitate viral attachment to the target cell surface. The consequent viral entry depends on S protein priming. As far as SARS-CoV is concerned, the entry receptor for S protein is angiotensin-converting enzyme 2 (ACE2) and the S protein priming is done by a cellular enzyme called transmembrane protease serine 2 (TMPRSS2). Since SARS-CoV and SARS-CoV-2 share about 76% amino acid similarity, a team affiliated with German, Austrian and Russian institutes hypothesized that SARS-CoV-2 cell entry would also depend on ACE2 and TMPRSS2.

|
|
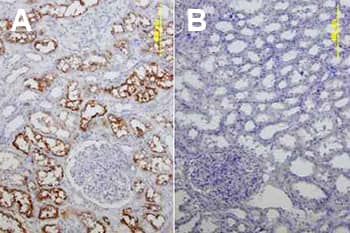
(Left) Western blot detection of ACE-2 in tissue lysates of human ovary, human testis, and human kidney. Goat Anti-Human ACE‑2 Polyclonal Antibody (Catalog AF933) was used at 1 µg/mL to probe the PVDF membrane and was followed by HRP-conjugated Anti-Goat IgG Secondary Antibody (Catalog HAF019). Analysis was conducted under reducing conditions. (Right) Immunohistochemical detection of ACE‑2 in immersion fixed paraffin-embedded sections of human kidney. (A) Goat Anti-Human ACE‑2 Polyclonal Antibody (Catalog AF933) was used at 15 µg/mL for overnight incubation at 4 °C followed by staining with Anti-Goat HRP-DAB Cell & Tissue Staining Kit (brown; Catalog CTS008) and counterstaining using hematoxylin (blue). (B) Omission of the primary antibody and tissue staining only with secondary antibody and detection reagents. |
|
Indeed, SARS-CoV-2 was found to use the same mechanism. That is, SARS-CoV-2 uses ACE2 for entry and TMPRSS2 primes the viral S protein. Investigators used ACE-2 polyclonal antibody (Catalog AF933) at 2 or 20 mg/mL to block SARS-S- and SARS-2-S- driven entry into Vero cells. Interestingly, a clinically used TMPRSS2 inhibitor, camostat mesylate , was found to block SARS-CoV-2 entry into the target cells.
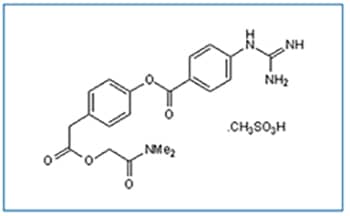 Camostat mesylate is an orally active protease inhibitor which inhibits transmembrane serine protease TMPRSS2 and partially blocks entry of SARS-Cov-2 (COVID-19) into lung cells in vitro.
Camostat mesylate is an orally active protease inhibitor which inhibits transmembrane serine protease TMPRSS2 and partially blocks entry of SARS-Cov-2 (COVID-19) into lung cells in vitro.
This means that there is a glimmer of hope, but only time will tell if blocking viral entry by inhibiting TMPRSS2 is a viable strategy for treating COVID-19. However, the fact that the infection mechanism is similar to SARS-CoV may provide a significant step forward in identifying effective strategies to battle this new threat.
Find SARS-CoV-2 Research Resources »
 Jamshed Arslan, Pharm D, PhD
Jamshed Arslan, Pharm D, PhD
Dr Arslan is an Assistant Professor at Barrett Hodgson University, Pakistan,
where he uses various pedagogical methods to teach Pharm D students.
Research in focus
Hoffmann M, Kleine-Weber H, Schroeder S, et al. (2020). SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clinically Proven Protease Inhibitor. Cell, S0092-8674(20)30229-4. doi:10.1016/j.cell.2020.02.052